Dry Eye
Written by Jane Wolford, O.D.
What is dry eye?
Dry eye occurs when the quantity and/or quality of tears fails to keep the surface of the eye adequately lubricated. Dry eye affects millions of adults in the United States. The risk of developing dry eye increases with advancing age and women have a higher prevalence of dry eye compared with men.
What are the symptoms of dry eye?
Dry eye causes a scratchy sensation or the feeling that something is in the eye. Other symptoms include stinging or burning, blurred vision, episodes of excess tearing that follow periods of dryness, discharge, pain, and redness in the eye.
What are tears and how do they relate to dry eye?
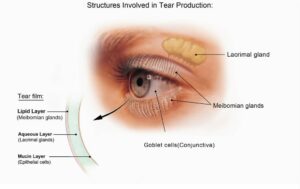
In a healthy eye, lubricating tears called basal tears continuously bathe the cornea, the clear, outer surface of the eye. With every blink of the eye, basal tears flow across the cornea, nourishing its cells and providing a layer of liquid protection from the environment. When the glands nearby each eye fail to produce enough basal tears, or when the composition of the tears changes, the health of the eye and vision are compromised. Tears are a complex mixture of fatty oils, water, mucus, and more than 1500 different proteins that keep the surface of the eye smooth and protected from the environment, irritants, and infectious pathogens. Tears form in three layers:
- An outer, oily (lipid) layer, produced by the Meibomian glands, keeps tears from evaporating too quickly and helps tears remain on the eye.
- A middle (aqueous) layer contains the watery portion of tears and water-soluble proteins. This layer is produced by the main lacrimal gland and accessory lacrimal glands. It nourishes the cornea and the conjunctiva, the mucous membrane that covers the entire front of the eye and the inside of the eyelids.
- An inner (mucin) layer, produced by goblet cells, binds the aqueous layer to ensure that the eye remains wet.
What causes dry eye?
Dry eye can occur when basal tear production decreases, tear evaporation increases, or tear composition is imbalanced. Factors that can contribute to dry eye include the following:
- Medications: antihistamines, decongestants, antidepressants, birth control pills, hormone replacement therapy, medications for anxiety, Parkinson’s disease, and high blood pressure have been associated with dry eye.
- Advancing age as there is a decline in tear production. Dry eye is more common in people age 50 years or older.
- Rosacea (an inflammatory skin disease) and blepharitis (an inflammatory eyelid disease) can disrupt the function of the Meibomian glands.
- Autoimmune disorders: Sjögren’s syndrome, lupus, scleroderma, rheumatoid arthritis, diabetes, thyroid disorders, and Vitamin A deficiency are associated with dry eye.
- Women are more likely to develop dry eye. Hormonal changes during pregnancy and after menopause have been linked with dry eye as well as an increased risk for autoimmune disorders.
- Windy, smoky, or dry environments increase tear evaporation.
- Seasonal allergies can contribute to dry eye.
- Prolonged periods of screen time encourage insufficient blinking.
- Laser eye surgery may cause temporary dry eye symptoms.
How is dry eye diagnosed and treated?
People experiencing dry eye symptoms should schedule a dry eye consultation with our office to determine the cause, which guides treatment strategy.
Over-the-counter (OTC) topical medications. Mild dry eye symptoms may be treated with over-the-counter medications such as artificial tears, gels, and ointments.
Environmental and lifestyle changes. Cutting back on screen time and taking periodic eye breaks may help. Closing the eyes for a few minutes, or blinking repeatedly for a few seconds, may replenish basal tears and spread them more evenly across the eye. Sunglasses that wrap around the face and have side shields that block wind and dry air can reduce symptoms in windy or dry conditions.
Smoking cessation and limiting exposure to secondhand smoke will help.
Prescription dry eye medications. Cyclosporine and lifitegrast are the only prescription medications approved by the U.S. Food and Drug Administration for treating dry eye. Corticosteroid eye drops also may be prescribed short-term to reduce eye inflammation.
Devices. FDA-approved devices provide temporary relief from dry eye by stimulating glands and nerves associated with tear production. Our office is pleased to be one of the first offices to be working with True Tears™.
Surgical options. Punctal plugs made of silicone or collagen may be inserted by an eye care professional to partially or completely plug the tear ducts at the inner corners of the eye to keep tears from draining from the eye. In severe cases, in-office surgical closure of the drainage ducts.
Nutritional Support
Dietary support including the addition of Omega 3 and the anti inflammatory Omega 6 supplements as well as decreasing processed foods.
Upcoming research
NEI-supported researchers are studying the underlying causes of dry eye to better understand the disease and to develop novel treatments.
In a healthy eye, only one-tenth of a degree of cooling from evaporation is needed for activation of nerves that trigger basal tearing. Researchers are investigating factors that influence the ability of corneal nerves to sense tear evaporation. Such research may lead to the development of topical corneal nerve stimulators, or products that increase nerve sensitivity to drying.
The protein lacritin in tears promotes basal tearing (via nerve stimulation) and eye health. Some people with dry eye have low levels of lacritin in their tears. A topical, synthetic form of the protein has been developed for initial testing in people with dry eye.
Since corneal nerve number, length, and function are substantially diminished in dry eye, another research goal is to devise ways to promote their regrowth. Such a product could also help individuals suffering from dry eye after corneal laser surgery, such as LASIK.
Other research is exploring the role of stem cells in the natural development of lacrimal glands. This early-stage research may eventually enable use of a patient’s own stem cells to rebuild or replace tear-producing lacrimal glands.
Investigation is ongoing into the molecular composition of the tear lipid layer, and factors that either stabilize or destabilize it. Treatments to stabilize it may help reduce tear evaporation.