Diabetes is a chronic health condition that affects your body’s ability to create and/or utilize insulin. Insulin is the trigger for glucose, derived from the food we eat, to be allowed into our cells and used as energy. Without the correct amount of insulin, our cells don’t absorb that glucose and it remains in our blood. According to the Mayo Clinic, a surplus of blood sugar in our bodies over time can lead to cardiovascular disease, nerve damage, kidney damage, foot damage, and skin infections.
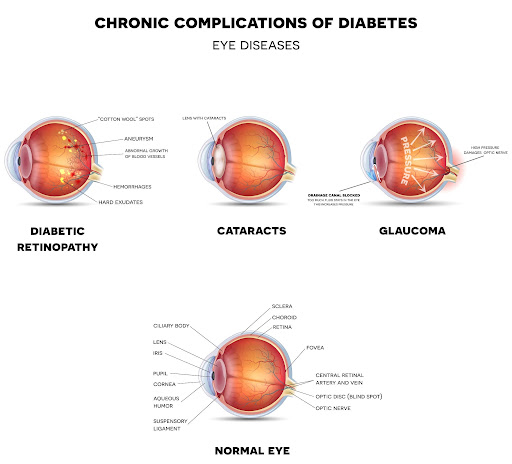
In addition, diabetes can have a severe impact on your vision. Diabetic eye disease is defined by the National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK) as a “group of eye problems” including “diabetic retinopathy, diabetic macular edema, cataracts, and glaucoma.”
Here we will discuss the effects that diabetes and diabetic eye disease have on your sight. However, the first line of defense if you suffer from diabetes, have a family history of diabetes, or are prediabetic is to make an appointment with your general practitioner and your eye doctor.
Short Term Effects of Diabetes
Even in the short term, diabetes can have an effect on your vision. “High glucose can change fluid levels or cause swelling in the tissues of your eyes that help you to focus, causing blurred vision,” according to NIDDK. Though temporary, this blurred vision can last anywhere from a few days to a couple of weeks, but will typically dissipate when your blood sugar comes within a normal range.
Effects of Diabetic Eye Diseases
Diabetic Retinopathy
Diabetic retinopathy is a result of high blood sugar over time. Too much sugar in the blood leads to blockage of the blood vessels that nourish the retina, which cuts off its blood supply. As a result, the eye attempts to grow new blood vessels, but those new blood vessels don’t develop properly and leak easily. When they leak, you can develop black spots in your vision and if the leak (or bleed) is heavy, your vision can be blocked entirely. In fact, diabetic retinopathy is the number one cause of legal blindness in the country for patients under 64.
Can it be prevented?
The Centers for Disease Control and Detection (CDC) assert that, “Early detection and treatment can prevent or delay blindness due to diabetic retinopathy in 90% of people with diabetes.” By getting a dilated eye exam once a year, it is possible to detect an issue before damage can be done.
Symptoms
Symptoms of diabetic retinopathy are largely absent in the early stages. The American Academy of Ophthalmology states that as the condition worsens, you might notice:
- Floaters
- Blurry vision
- Blank or dark spots in your vision
- Difficulties with night vision
- Loss of vision
- Colors seeming faded
Treatment
Treatment options for diabetic retinopathy include stabilizing your blood sugar and blood pressure, medicine, eye injections, and laser surgery.
Diabetic Macular Edema
The central portion of the retina, the macula, is responsible for our sharpest central (reading) vision. Small blood vessels travel through the retina supplying it with oxygen and removing waste products. Diabetic macular edema is caused by fluid leaking from the retinal blood vessels into the surrounding retina, causing it to become swollen and distorted.
Can it be prevented?
The accumulation of fluid in the macula is present in about 9% of all diabetics. The likelihood of developing macular edema increases as a person has diabetes for a longer period of time. Many physicians feel that high blood pressure, abnormal kidney function, and other general systemic factors may contribute to the problem of diabetic macular edema. It is therefore important to have the best possible control of blood pressure, kidney function, and levels of sugar when treating macular edema.
Symptoms
The only symptom of macular edema is decreased vision. However, it usually develops in patients that have shown other signs of diabetic eye disease. Since there are many other causes of decreased vision in diabetics, an examination by an ophthalmologist is the only way to determine if a particular person has macular edema.
Treatment
Treatment of macular edema is possible with laser therapy or medications injected into the eye. However, the main goal of laser treatment is to stop any further deterioration, not to repair your vision. Make sure to contact your ophthalmologist at the first sign of any vision issues in order to catch and treat the macular edema as early as possible. Then your ophthalmologist will use a fluorescein angiogram to help determine the best way for the treatment to be applied.
Cataracts
According to NIDDK, “The lenses within our eyes are clear structures that help provide sharp vision—but they tend to become cloudy as we age.” That cloudiness is called cataracts and they are the leading cause of blindness worldwide.
Most cases of cataracts occur in people over the age of 40 and are due to aging or injury. However, people with diabetes tend to develop cataracts at an earlier age. It is thought that the high blood glucose levels in people with diabetes can create deposits of proteins on the lens. Cataracts will develop in both eyes, but not necessarily at the same rate.
Can it be prevented?
There is no clear strategy for preventing cataracts. Yet there are several factors that doctors believe could help.
- Schedule regular eye exams
- Keep other health problems (diabetes) under control
- Quit smoking
- Limit your consumption of alcohol
- Maintain a healthy diet
- Wear sunglasses
Symptoms
Cataracts develop slowly and sometimes you won’t notice a change in your vision right away. This is all the more reason to schedule regular eye exams. If you do notice any of the following symptoms listed by the Mayo Clinic, be sure to contact your ophthalmologist immediately.
- Clouded, blurred or dim vision
- Increasing difficulty with vision at night
- Sensitivity to light and glare
- Need for brighter light for reading and other activities
- Seeing “halos” around lights
- Frequent changes in eyeglass or contact lens prescription
- Fading or yellowing of colors
- Double vision in a single eye
Treatment
First, your doctor will attempt to remedy the effects of your cataracts by increasing your glasses prescription. However, if the cataracts worsen, inhibiting your daily life, you may need surgery to remove the clouded lens and replace it with an artificial lens.
Glaucoma
Glaucoma is a complex disease in which damage to the optic nerve leads to progressive, irreversible vision loss and blindness. Though we are not sure exactly what causes glaucoma, it seems to be a result of elevated intraocular pressure. A diabetic’s likelihood of developing glaucoma is twice that of someone without diabetes. If left untreated, blindness is inevitable.
Can it be prevented?
Glaucoma is often referred to as a “silent thief” of sight because of the lack of noticeable symptoms in the early stages. The only way to prevent further deterioration from glaucoma is by having a comprehensive dilated eye exam every 1-2 years. Once glaucoma is detected, you need to take steps to lower the eye pressure as soon as possible because vision loss due to glaucoma cannot be recovered.
Symptoms
Early symptoms of glaucoma are subtle losses of peripheral vision that often go completely unnoticed. As the disease progresses you’ll observe:
- Blurred vision
- Eye pain
- Headache
- Halos around lights
- Peripheral vision loss
- Tunnel vision
- Eye redness
- Hazy-looking eye
- Nausea
Treatment
When choosing the best course of treatment for glaucoma we consider the kind of glaucoma you have, the stage of the disease, and your lifestyle. In many cases, we begin medical therapy with eye drops. These can help decrease eye pressure by improving how fluid drains from your eye or by decreasing the amount of fluid your eye makes. We monitor the responsiveness and make changes depending on eye pressure and visual field changes.
If the eye drops aren’t effective enough, we can use a laser trabeculectomy to lower the intraocular pressure by making a small hole in the eye wall (sclera), covered by a thin “trap-door”. This lets fluid leak from inside the eye, out through the wall of the eye, and under the covering tissue where it is slowly absorbed.
When medications and/or laser treatment are unable to reduce the eye pressure enough, the best choice is to surgically insert a tube shunt, a flexible plastic tube with an attached silicone drainage pouch, in the eye to help drain fluid from the eye.
What can you do to protect your vision?
The best way to protect your vision is to manage your diabetes and to mention any visual symptoms you may have to your doctor immediately. Diabetic eye diseases are complex problems that require continued observation and care under the supervision of your ophthalmologist and personal physician.
You need the comfort of knowing you are working with a doctor or surgeon that understands your condition, is highly trained in your specific area of need, and is current on all of the latest technology and research. At the Eye Care Center of Northern Colorado, you can expect the highest level of care and expertise. Our specialists will work with you to figure out your best options.
To schedule your Longmont, Lafayette, Greeley, or Boulder eye exam, contact us today!
For more information on eye health, see our blogs on Common Retinal Disorders and The Basics of Maintaining Good Eye Health. Also peruse our page on Diabetic Eye Disease and listen to Dr. Justin M. Kanoff in his video on Diabetic Disease Treatment. In addition, our Patient Education Portal has a wealth of information on a variety of eye-related topics!
Resources and References-
Diabetic Eye Disease:
https://www.aao.org/eye-health/diseases/diabetic-eye-disease
https://www.mayoclinic.org/diseases-conditions/diabetes/symptoms-causes/syc-20371444
Diabetic Retinopathy:
https://www.aao.org/eye-health/diseases/what-is-diabetic-retinopathy
https://www.cdc.gov/visionhealth/resources/features/keep-eye-on-vision-health.html
Diabetic Macular Edema
https://eyecaresite.com/eye-care/common-eye-disorders/diabetic-eye-disease/
Cataracts
https://www.mayoclinic.org/diseases-conditions/cataracts/symptoms-causes/syc-20353790
Glaucoma
https://www.nei.nih.gov/learn-about-eye-health/eye-conditions-and-diseases/glaucoma
https://eyecaresite.com/multispecialty-eye-surgery/glaucoma/symptoms-of-glaucoma/